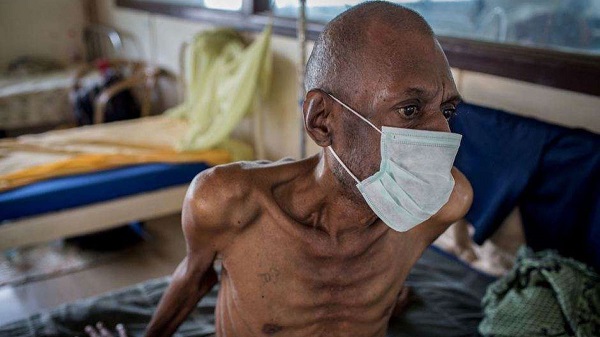
Lola was a tuberculosis (TB) patient who had also tested positive for HIV. Rapid diagnostic tests showed that she had multi-drug resistant (MDR) TB. This means that the first-line drugs were not effective for her treatment. Hence, second-line drugs were prescribed for her. Her family wondered why her health worsened speedily and her doctors were baffled that the other drugs were not effective for her. She died of complications from TB and HIV.
Lola was one of the Nigerians for whom the drug resistance of the bacteria that caused her TB was misdiagnosed. This is according to research published by scientists at the African Centre of Excellence for Genomics of Infectious Diseases (ACEGID) and their partners, using next-generation sequencing (NGS). The scientists discovered that Lola had extensively drug-resistant (XDR) TB.
“We used genome sequencing to give the full profile of some samples that were classified as drug-resistant and multi-drug resistant. And the sequencing results gave us the understanding that these samples were extensively drug-resistant TB,” said Idowu Olawoye, the first author of the paper and a PhD Research Fellow at ACEGID.
“That shows us how often cases like this can be missed. When people go to the hospitals to treat TB, the clinics would give them drugs that would not make them feel better or kill the bacteria because the bacteria is resistant to that drug,” he continued.
Tuberculosis is an infectious disease caused by the bacteria Mycobacterium tuberculosis (the TB bacteria). It typically affects the lungs, as well as other parts of the body. Symptoms of the disease include a persistent cough that lasts more than three weeks (the phlegm of which can be bloody), weight loss, night sweats, high temperature, tiredness and fatigue, among others.
As with other disease-causing microorganisms, the TB bacteria expresses changes (mutations) in its genetic material. These changes help it to withstand the drugs used against it. The nature and extent of these changes determine if individual drugs can successfully treat TB in patients. Hence, the evolution of the different classes of drug-resistant TB.
The XDR TB is a rare type of multi-drug resistant TB, which is resistant to two of the most important, first-line drugs (Rifampicin and Isoniazid) used to treat TB. The XDR TB bacteria have mutations (genetic changes) that help them resist all first-line anti-TB drugs, at least one second-line medication and at least one third-line drug.
Next-generation sequencing is an advanced DNA sequencing technology that involves simultaneous sequencing of multiple, small fragments of DNA to determine the sequence of an organism’s genome. With NGS, scientists can determine the order of nucleotides in the entire genome or portions of DNA/RNA.
When TB patients breathe, speak and cough, droplets containing the tuberculosis bacteria are released into the air from their lungs or throat. Healthy individuals get infected when they breathe in these bacteria. This shows the ease with which the disease can spread and why resistance misdiagnosis is dangerous.
“When you misdiagnose a patient with drug-resistant tuberculosis, it is a major problem, not just in the local community but globally,” said Dr. Nike Arawomo, Consultant Pulmonologist at the Obafemi Awolowo University Teaching Hospital Complex, Ile-Ife. “It means that the patient will be treated as a regular TB patient. When those patients are treated so because they are not getting the right drugs, they do not respond to the treatment you are giving and they are likely going to die from the disease.”
This was the case with Lola.
Treatment of drug-resistant TB is different from that of non-resistant TB in terms of drug administered, the intensity (quantity) and how long the patient is required to take the drugs. Drugs administered to patients with drug-resistant TB usually have more side effects and a deeper impact on patients’ quality of life. Hence, it is important to correctly diagnose the drug-resistant type in patients.
Unfortunately, Bala’s story highlights how misdiagnosis can affect patients and lead to greater TB spread. Just like Lola, Bala was also diagnosed with Rifampicin-resistant TB. Hence, second-line TB drugs were prescribed for him. He took the drugs for a while but stopped. Why? The drugs had severe side effects on him and there was no marked improvement in his health. The recent study using NGS, however, showed that he had XDR TB. He would have continued to infect others with this strain of drug-resistant TB.
Both Bala and Lola lived in Lagos, Nigeria’s commercial capital with a population of over 20 million people. Misdiagnosis of the TB strain that infects patients can severely impede efforts to contain and eliminate TB in the country.
In 2019, Nigeria carried the sixth-largest burden of TB in the world, accounting for an estimated 440,000 TB cases, according to the World Health Organization’s Global Tuberculosis Report, 2020. This calls for a closer look at how TB is managed in the country.
“For surveillance purposes, I think NGS is the way to go because it will not only enable you to identify established markers of MDR. It will also enable you to discover novel mutations that could be associated with extremely resistant organisms, like the ones we found,” said Prof. Christian Happi, Director of ACEGID.
“Tuberculosis is a treatable disease. No one should die from tuberculosis,” concluded Arawomo.
“Anybody that has been coughing for over two weeks should come to the hospital where we will conduct a test. Once they do this, we pick it (TB) early and we start them on the appropriate drug. TB drugs are free.”
As we mark the World Antimicrobial Awareness Week 2021, it is important to strengthen the TB surveillance system in Nigeria. Incorporating next-generation sequencing into the system will help accomplish this.
Fikayo Oyewale is the Scientific Communications Officer, African Centre of Excellence for Genomics of Infectious Diseases, Redeemer’s University, Ede, Osun State.

