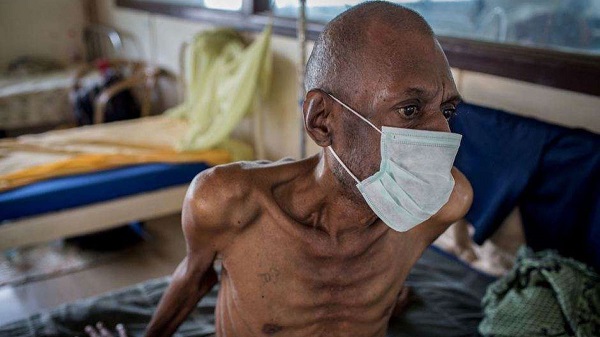
Mr. Isah Dogara, from Iowa community in the Federal Capital Territory, about 35km from Gwagwalada, said his macho attitude and belief in traditional medicine led to him infecting his wife and late mother with tuberculosis (TB) – all because he feared that being diagnosed with the disease would make him vulnerable.
Dogara, a 39-year-old miner, believed he was cursed when he started coughing and preferred to take ‘Baban Aisha’, a popular traditional remedy. Even though the cough worsened, he delayed seeking medical care because he was told to give the medication some time to cure his uncontrollable cough.
“I failed to recognise my symptoms were due to TB, which I called an ‘ordinary cough’. See, it has kept me down for over two years,” he said. “I finally reported at the Gwagwalada [Specialist] hospital only after a prolonged period of self-medication with ‘Baban Aisha’.
“When I finally made up my mind to go to the hospital, it was after nine appointments with the doctors (that) I was finally diagnosed with TB. My cousins, with whom I work, doubted the diagnosis and advised me to go for a traditional medication better than the Baba Aisha I took earlier.
“What my cousin claimed worked for other colleagues who were also coughing almost ended my life when I saw myself in the hospital,” he added.
Dogara said his wife and his late mother became infected, but never showed any symptoms of TB, adding: “But my mother died from co-morbidity of diabetes and high blood pressure while being treated for TB.”
According to the World Health Organisation (WHO), TB is the 13th leading cause of death globally and the second leading infectious killer after COVID-19 and HIV/AIDS.
In 2020 about 6 in every 10 persons infected with TB were male, with an estimated 10 million people (5.6 million men, 3.3 million women and 1.1 million children) testing positive.
A total of 1.5 million people were lost to TB in the year. TB is an infectious disease caused by mycobacterium tuberculosis bacteria and affects the lungs of sufferers; it is curable and preventable. As an airborne disease, it spreads through cough, sneezing or saliva. The disease affects all age groups.
Fear of the social stigma associated with a TB diagnosis makes men delay getting tested for the disease.
In some cases, when married men test positive for TB, they may withhold the information from their family, increasing the likelihood of spreading the disease to their partners and children, who could otherwise have taken preventive action.
In most cases, TB is curable – if the right treatment is available. However, drug-resistant TB is becoming more prevalent and can be fatal.
Such was the case of 54-year-old Paula Bitrus, a resident of Abaji, FCT. The former class teacher was diagnosed with multi-drug resistant TB (MDR-TB) and HIV and spent more than 21 months caring for her paralysed husband who refused to go to the hospital, because of the stigma associated with TB. He later died of both ailments.
Bitrus contracted the disease from her husband who hid his diagnosis from her and never sought medical attention because he was an elder in the church and concerned about a possible loss of status.
“He died from the ‘what will people say?’ syndrome. He was afraid of getting a ‘back’ seat in church and he died from inflammation in his lungs induced by severe coughing,” she said.
In such cases, lung function is severely diminished and results in breathlessness.
“The bacteria induce fevers and sweats, particularly at night. We suffered. No drugs were working and accessing TB drugs without being registered in any of the health facilities was impossible. Eventually, blood vessels feeding the lungs rupture, further diminishing functions and contributing to increasing anaemia. He suffered before he finally died from pride and ego,” she narrated.
The lack of knowledge of health care workers in managing TB cases and poor interpersonal relations and communication with people who have TB have negative effects on men who are expected to adhere to the long treatment schedule for TB.
Mr. Khali Adamu of Bwari local government area in the FCT, narrates his experiences as an ex-convict: “I remember how I got a cough, accompanied by catarrh and high fever. It ended up being a TB infection. Despite the free treatment I was told was available, I ran away from the Dantsoho Memorial Hospital, Kaduna, to Abuja, just because of isolation and maltreatment from health workers.
“I was poorly counselled on TB and my treatment ended up [yielding] poor outcomes because the health workers threw my drugs at me and put my food by the door. I was not examined while I was there; they only asked me how I was feeling from afar. [Most times] they did so by speaking through the window.
“Such experience never gave me hope in the treatment, so I stopped it. Sometimes, I could not speak because of the pains I felt around my neck and chest and they continued taunting me, asking me to ‘be a man’. This was why I ran away. “When I got to Abuja, I met an NGO that helped me better understand what I was feeling and how important it was for me to seek medical attention. That was the turn-around for me,” he added.
Adamu, already diagnosed with sickle cell disease, had fluid building up in his lungs – a symptom typically associated with severe and long-term TB infections.
The idea of men being more resilient to illness also appears to be linked to the perception of the illness and its severity. Men described a pattern of waiting to see if their conditions would improve before seeking out care and only going to formal healthcare when the illness was at an advanced stage.
Meanwhile, according to Dataphyte, 30 countries are considered ‘high burden TB countries’ as they accounted for 86 per cent of the new cases in 2020. Eight of these countries accounted for two-thirds of the total cases. India topped the list followed by China, Indonesia, the Philippines, Pakistan, Nigeria, Bangladesh and South Africa.
Continued investment in the fight against TB saw global cases fall by 2 per cent between 2015 and 2020. However, it is expected that $13 billion will be needed in 2022 to combat the scourge effectively.
It said the cost of treatment remains out of reach for those infected, as one in two TB-affected households spends more than 20 per cent of their household income on treatment.
Dataphyte said that the TB caseload in Nigeria was attributed to five high-risk factors in 2020. The leading factor is undernourishment, followed by HIV, diabetes, smoking and alcohol use.
It said treatment coverage was poor in the country, as only about 30 per cent of TB cases were treated in 2020.
“This is a fall from the treatment success recorded in 2019, as it recorded an 88 per cent treatment success rate covering 117,150 cohorts. Thus, Nigeria is among the 10 countries with the largest gap between notifications of new and relapse cases, as well as the best estimates of TB incidence,” it stated.
Mrs. Ekezie Eugenia, a focal person for drug resistance persons in Imo State, stressed the differences in men’s health-seeking behaviour.
“Men have a higher prevalence of undiagnosed TB than women and can spend up to a year longer contributing to ongoing transmission in the community before receiving treatment.
“Health workers find it difficult to enrol men for treatment once they were diagnosed,” she said, adding that some abscond even after they begin treatment.
“Health outcomes are often worse for patients with TB living in informal settlements, especially men,” Eugenia said. “In this job, I am yet to see a man who does not complain about the duration of treatment. They easily believe that TB is not caused by bacteria, but by poisoning and witchcraft.
“The consequence of men delaying seeking medical care, or keeping information from health workers can be dire. This is the number one problem that leads them to miss the early signs of a more serious condition like TB. Especially when it comes to ‘silent symptoms’.”
Dr. Akyala Ishaku, a senior lecturer in the department of microbiology, Nasarawa State University, said that men diagnosed with TB at an early stage have a much better prognosis than those who show up too late to health facilities.
“By putting those exams off, male patients find themselves in much worse conditions. Many men convince themselves that their condition will improve on its own, not wanting to ‘bother’ a doctor because vulnerability sucks and they see going to the health facility as a weakness. Some have the ‘superhero syndrome’. Some men see themselves as forever strong and capable of handling anything,” he explained.
Ishaku stressed that opting for traditional healing also prevented many men from accessing health care facilities too.
“A major challenge that stops some men from visiting the hospital is belief in traditional medicine. Some men trust traditional medicine and oppose seeking treatment from healthcare facilities,” he said.
On the other hand, some health experts think that in terms of healthcare, women and children are given special treatment, while men are left out. They believe that without the inclusion of men and boys in healthcare programmes, as well as greater recognition of how gender, a lack of awareness and poverty intersect to prevent diagnosis and treatment of TB, efforts to end this deadly disease will continue to be hindered.
According to Dr. Bethrand Odume, country director of the KNCV Tuberculosis Foundation Nigeria, there is a need for the government to improve men’s pathways to care. Odume said this would require interventions that consider contextual issues by addressing individual-level socioeconomic factors and broader structural factors of gender-related social dynamics, as well as the health system throughout the country.
He said that TB is perceived and experienced as a virulent disease that hampers independent functioning, and whose treatment drains financial resources.
He called on the government to bring about interventions that would engage men with TB; a system that would include social protection mechanisms and promotion of wellness in the workplace (especially highlighting the importance of early diagnosis and treatment).
“Engaging the private and informal sectors in the improvement of quality of TB care in these sectors is critical to helping us to find the ‘missing patients’ (including men) with TB,” he advised.
The director, National Tuberculosis, Buruli Ulcer and Leprosy Control Programme (NTBLCP), Dr. Chukwuma Anyaike said stigma affects men’s health-seeking behaviour in the country and is a factor that drives the global burden of TB.
According to him, stigma does not only harm men affected by TB, it also reduces healthcare workers’ commitment to high-quality health care service delivery in the country. “Excessive stress, with probable undernutrition,” he said “give room to TB infection”.
He explained that, as breadwinners, men are constantly exposed to environmental hazards that favoured TB infection.
He cautioned against lifestyles – smoking, and occupations such as mining, among others – that may be risk factors for developing TB.
Anyaike said that creating awareness and improved laboratory networks encouraged health-seeking behaviour among men and resulted in improved case detection.
“Government is improving the strategies toward TB case detection in the country; more men coming up with TB is just confirming the obvious. Government still maintains the equitable distribution of healthcare delivery in the country.”

